Gastroparesis Side Effects Lawsuit
In recent years, a number of new weight loss drugs have been introduced that may cause gastroparesis, including Ozempic, Wegovy, Rybelsus, and Mounjaro.
Also known as stomach paralysis, gastric stasis or a gastric obstruction, gastroparesis side effects cause severe pain and digestive complications by impeding the normal movement of the stomach muscles. This often results in persistent vomiting and hospitalization, and can cause long-term health consequences.
Although the drug makers knew or should have known that the mechanism of action for these drugs may leave some users with painful and debilitating gastrointestinal side effects, a desire for profits was placed before the safety of consumers.
According to allegations raised in a growing number of gastroparesis lawsuits against Ozempic, Wegovy, Rybelsus and Mounjaro manufacturers, false and misleading information about the stomach risks has been provided to users and the medical community. As a result financial compensation may be available through a gastroparesis settlement.
Who Qualifies For A Gastroparesis Side Effects Lawsuit?
Ozempic lawsuits, Wegovy lawsuits and Mounjaro lawsuits are now being pursued against the manufacturers of these weight loss and diabetes drugs, claiming the companies failed to adequately research the potential gastroparesis side effects or warn that users may experience;
- Excessive vomiting
- Severe diarrhea
- Severe abdominal pain
- Gastrointestinal burning
- Other gastrointestinal injuries
Gastroparesis Side Effects Info On This Page
What is Gastroparesis?
What Causes Gastroparesis?
What are the Symptoms of Gastroparesis?
How Gastroparesis Side Effects Impact Diabetics
How is Gastroparesis Diagnosed?
What Medical Tests are Used to Diagnose Gastroparesis?
Is Gastroparesis Permanent?
Gastroparesis Treatment Options
Gastroparesis Lawsuits Against Ozempic, Wegovy, Rybelsus and Mounjaro
What is Gastroparesis?
Gastroparesis, often referred to as stomach paralysis or gastric obstruction, is a medical condition characterized by a significant delay in the movement of food from the stomach to the small intestine. Under typical circumstances, once food is consumed and swallowed, it reaches the stomach and muscular contractions break the undigested food down into smaller fragments.
These stomach contractions then propel the food forward into the small intestine, where further digestion and nutrient absorption takes place.
In individuals with gastroparesis, stomach muscle contractions become weak and may stop moving forward through the gastrointestinal tract entirely. As a result, the stomach is unable to efficiently empty its contents into the small intestine. This is known as delayed gastric emptying, and can lead to food remaining in the stomach for much longer than usual.
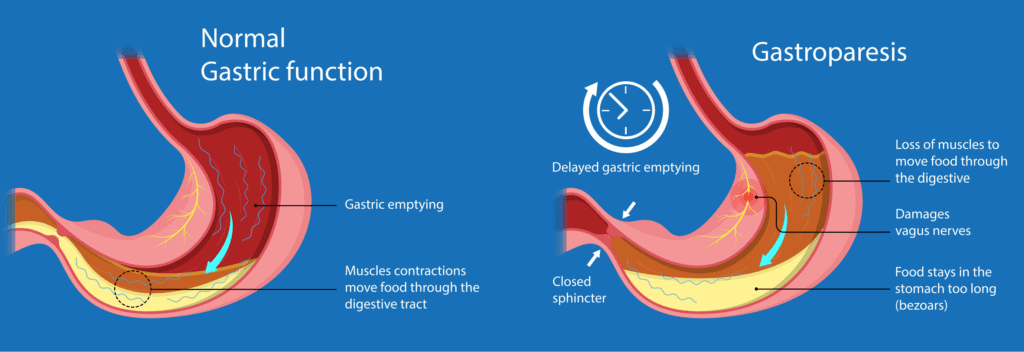
What causes gastroparesis?
Gastroparesis can arise from a variety of underlying causes, many of which relate to damage or dysfunction of the nerves or muscles controlling stomach motility. Although its exact cause might be unknown in several instances, numerous identifiable factors play a role in onset of the condition. Recognizing the root cause is pivotal for determining the most effective therapeutic approach and management plan.
Causes of Gastroparesis
- GLP-1 Medications: Medications such as Ozempic, Wegovy, Rybelsus and Mounjaro that are used for diabetes and weight loss can affect stomach motility and cause gastroparesis.
- Diabetes: Persistently elevated blood sugar levels can harm the vagus nerve that directs stomach muscle actions.
- Surgical injury: Operations involving the stomach or the vagus nerve might inadvertently damage them, resulting in gastroparesis.
- Viral infections: Some viruses have the potential to incite gastroparesis symptoms.
- Nervous system diseases: Afflictions like Parkinson’s disease and multiple sclerosis can have gastroparesis as a symptom.
- Connective tissue disorders: Illnesses such as scleroderma can influence stomach muscle function.
- Hypothyroidism: A sluggish thyroid can impede stomach emptying.
- Unknown causes: Often labeled as idiopathic gastroparesis, in these cases, the exact cause remains elusive.
How common is gastroparesis?
According to recent research published in 2023, Gastroparesis is relatively uncommon in the United States, with approximately 9.6 cases per 100,000 person-years for men and 37.8 cases per 100,000 person-years for women. However, its symptoms, similar to other gastrointestinal issues, are experienced by about 1 in 4 adults in the U.S.
What are the Symptoms of Gastroparesis?
Gastroparesis is a complex and often debilitating condition marked by a constellation of symptoms that can significantly impair the quality of life. These symptoms arise due to the stomach’s inability to empty its contents effectively, often without a clear mechanical obstruction.

Common Signs and Symptoms of Gastroparesis
- Nausea and Vomiting: One of the primary indicators of gastroparesis is persistent nausea, often aggravated after meals. This can be accompanied by bouts of vomiting, especially post-consumption.
- Feeling Full Quickly: An early satiety is common, where patients report feeling unusually full after ingesting only minimal quantities of food. This often leads to a decrease in overall food consumption and unintentional weight loss.
- Bloating and Abdominal Distension: Individuals with gastroparesis frequently describe a sensation of bloating or a distended abdomen, creating discomfort and unease.
- Heartburn or Acid Reflux: The compromised ability of the stomach to empty its contents effectively can lead to the regurgitation of stomach acids into the esophagus. This reflux manifests as a burning sensation, commonly referred to as heartburn or gastroesophageal reflux disease (GERD )
- Fluctuations in Blood Sugar Levels: For those with diabetes, gastroparesis can be particularly challenging as it affects the digestion and absorption patterns of carbohydrates. This irregularity can lead to unpredictable blood sugar level swings.
- Malnutrition and Dehydration: In extreme cases, the cumulative impact of reduced food intake, frequent vomiting, and the body’s inability to absorb nutrients effectively can result in malnutrition. Additionally, persistent vomiting can lead to dehydration, necessitating medical intervention.
Bezoar Formation Due to GLP-1 Medications
Ozempic (semaglutide) is an example of a GLP-1 (glucagon-like peptide-1) receptor agonist. This class of medications works by mimicking the action of the body’s natural GLP-1 hormone, which in turn slows gastric emptying, improves the release of insulin in response to meals, and reduces the amount of glucose released by the liver.
When patients with gastroparesis are prescribed GLP-1 medications such as Ozempic, Mounjaro or Wegovy, there’s a compounded effect. The inherent slowed emptying from gastroparesis combined with the deliberate slowing caused by the medication dramatically increases the risk of bezoars. It is a compounded effect on the stomach’s ability to clear its contents.
What does a bezoar feel like? Symptoms vary depending on the size and location of the bezoar. Some individuals may not experience any noticeable symptoms, while others might experience:
- A feeling of fullness after eating a small amount of food.
- Nausea or vomiting.
- Pain or discomfort in the stomach or abdomen.
- Bloating or a feeling of heaviness in the stomach.
Complications of Bezoars:
- Blockage: A bezoar can obstruct the gastrointestinal tract. Depending on its size and location, it can prevent the passage of food and liquid. This can result in severe abdominal pain, vomiting, and in critical situations, can hinder blood flow to the affected part of the digestive system.
- Ulcers: If a bezoar stays in one place in the stomach for too long, it can cause pressure against the stomach lining, leading to ulcer formation. An ulcer is a sore or lesion that develops on the lining of the stomach or intestines.
- Bleeding: A progressed ulcer can lead to bleeding. Symptoms might include vomiting blood or passing black, tarry stools. This is a grave condition and necessitates immediate medical attention.
It’s essential for individuals on GLP-1 medications like Ozempic to be aware of these potential risks and consult with their healthcare provider if they experience any unusual gastrointestinal symptoms.
How Gastroparesis Side Effects Impact Diabetics
The slow movement of food through the stomach caused by gastroparesis can be problematic for diabetics, where precise timing of nutrient absorption and insulin administration is essential for blood sugar regulation.
When stomach paralysis is induced by a drug due to its disruption of hormone function, the complexities multiply. Let’s break down the implications of drug-induced gastroparesis in diabetics due to disrupted hormone function:
- Glycemic Control Issues: The most immediate concern for diabetics with gastroparesis is the unpredictable delay in food passing from the stomach to the small intestine. Normally, when food is ingested, carbohydrates are broken down into glucose, leading to a rise in blood glucose levels. Diabetics typically adjust their insulin dosage based on their carbohydrate intake. However, with gastroparesis, since food digestion and movement become unpredictable, there might be a mismatch between the amount of insulin administered and the amount of glucose entering the bloodstream. This can result in erratic blood sugar levels, causing both hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar).
- Disruption of Hormone Function: If a drug is the cause of gastroparesis due to its interference with hormone function, this adds another layer of complexity. Hormones play crucial roles in glucose metabolism. For instance, the hormone glucagon-like peptide-1 (GLP-1) stimulates insulin release and inhibits glucagon release (which raises blood glucose). If a drug disrupts this or other hormones, it could directly affect blood sugar control.
- Symptoms Exacerbation: Diabetics often experience complications like nerve damage. Gastroparesis, with its symptoms of nausea, vomiting, bloating, and abdominal pain, can exacerbate the discomfort and decrease the quality of life.
- Nutrient Absorption: Diabetics need to ensure they receive adequate nutrients to manage their condition and overall health. Gastroparesis can affect nutrient absorption due to inconsistent digestion or vomiting, which can have a cascading effect on overall health and the management of diabetes.
- Medication Absorption: Some oral diabetic medications may not be absorbed effectively if the stomach doesn’t empty properly. This can affect their therapeutic effectiveness.
- Higher Risk of Complications: Uncontrolled blood sugar due to gastroparesis can increase the risk of long-term diabetic complications, including kidney disease, retinopathy (eye disease), and further neuropathy.
How is Gastroparesis Diagnosed?
Gastroparesis from Ozempic, Wegovy or Mounjaro requires thorough examination for an accurate diagnosis. While the symptoms can be telling, a physician will take several steps to ensure they pinpoint the exact cause and rule out other potential health issues.
Medical Background Analysis
To understand the onset and progression of your symptoms, your doctor will conduct an in-depth review of your medical history. This involves:
- Symptom Analysis: A physician will want to understand the specifics of your current symptoms.
- Medication and Supplement Inquiry: Given that some drugs can impact gastric motility, it’s crucial to inform the doctor about all prescription medications, over-the-counter drugs, and any dietary supplements you’re currently taking.
- Past Health Concerns: Conditions such as diabetes, scleroderma, nervous system disorders, and hypothyroidism can be linked to gastroparesis, so it’s essential to discuss any history of these.
- Surgical and Treatment Background: The doctor will inquire if you’ve previously undergone surgeries involving your esophagus, stomach, or small intestine. Additionally, they’ll ask if you’ve had radiation therapy targeting your chest or stomach region.
Physical Exam
A physical examination is a crucial part of the diagnostic process. Here’s what your doctor will focus on:
- Vital Sign Monitoring: Checking your blood pressure, temperature, and heart rate will provide insights into your overall health.
- Dehydration and Malnutrition: Given that gastroparesis can lead to reduced food intake and frequent vomiting, your doctor will assess for signs of dehydration and malnutrition.
- Abdominal Check: Listening for unusual sounds and feeling the abdomen can reveal tenderness or pain, suggesting inflammation or other complications.
Following these procedures, the doctor might recommend blood tests and further medical tests, both to confirm the presence of gastroparesis and to exclude other conditions with similar symptoms.
What Medical Tests are Used to Diagnose Gastroparesis from Ozempic, Wegovy or Mounjaro?
Following hospitalization for gastrointestinal problems from Ozempic, Wegovy or Mounjaro, a doctor may perform one or more of the following tests to measure how fast your stomach is emptying its contents to diagnose gastroparesis.
Gastric emptying scan
Also called gastric emptying scintigraphy, the scan consists of a patient consuming a bland meal that contains a small amount of radioactive material. Afterward, a camera outside the body scans the abdomen to track the radioactive material, which provides a measure of how quickly the stomach empties its contents after the meal. If the stomach takes an unusually long time to empty, this is indicative of gastroparesis caused by Ozempic, Wegovy or Mounjaro.
Typically, the scan lasts about 4 hours. This test is considered the gold standard for diagnosing gastroparesis because of its accuracy and reliability.
Gastric emptying breath test
For this test, you eat a meal that contains a substance that is absorbed in your intestines and eventually passed into your breath. After you eat the meal, a health care professional collects samples of your breath over a period of a few hours—usually about 4 hours. The test can show how fast your stomach empties after the meal by measuring the amount of the substance in your breath.
Wireless motility capsule
Also known as a SmartPill, the wireless motility capsule is a small electronic device that you swallow. The capsule moves through your entire digestive tract and sends information to a recorder hung around your neck or clipped to your belt. A healthcare professional uses the information to find out how fast or slow your stomach empties, and how fast liquid and food move through your small intestine and large intestine. The capsule will pass naturally out of your body with a bowel movement.
Is Gastroparesis Permanent?
Gastroparesis, often termed “delayed stomach emptying,” can become a permanent condition in individuals who have suffered damage to their vagus nerve. The vagus nerve plays a critical role in regulating the muscular contractions of the stomach, facilitating the movement of food through the digestive system. When this nerve is damaged, it can lead to a disruption in these contractions, causing food to remain in the stomach for prolonged periods.
Despite various treatments that can help manage symptoms, if the root cause of the gastroparesis is irreversible damage to the vagus nerve, individuals may experience lifelong challenges associated with the condition.
How Long Does Gastroparesis Last After Stopping Ozempic?
Gastroparesis-like symptoms associated with Ozempic, Wegovy, Mounjaro and other GLP-1 receptor agonists may resolve after stopping use of the medications. However, case reports have shown that it may take months for symptoms to resolve, often resulting in multiple hospital visits, medical testing and the accrual of medical bills. If gastroparesis after Ozempic use results in nerve damage, former users may be left with permanent injuries.
According to a case report published in the Journal of Investigative Medicine in October 2021, a 52-year-old female taking semaglutide reported experiencing severe gastric pain, accompanied by fullness, bloating, and vomiting within one month of starting weekly injections. The individual underwent multiple tests including upper and lower endoscopies, a hepatobiliary iminodiacetic acid (HIDA) scan, abdominal Doppler blood flow study, as well as multiple medications to relieve the gastroparesis symptoms.
The case report indicates that no abnormalities were identified in the medical evaluations and symptoms only resolved after stopping the use of semaglutide. Researchers reported the symptoms subsided after six weeks of stopping semaglutide injections.
However, individuals have claimed their gastroparesis side effects did not resolve after stopping the medication, and have resulted in other permanent gastrointestinal injuries.
Gastroparesis Treatment Options
The method by which gastroparesis is treated is determined by its root cause, the intensity of symptoms, potential complications, and a patient’s response to distinct therapeutic strategies. Occasionally, addressing the underlying cause can alleviate gastroparesis.
Dietary Adjustments
Changing your eating habits can be an effective way to treat gastroparesis symptoms and ensure adequate nutrient, calorie, and fluid intake, which are essential in countering complications such as malnutrition and dehydration. Recommendations might include:
- Eating less fatty foods
- Steering clear of high-fiber foods.
- Consuming multiple small meals over fewer, larger ones.
- Thoroughly chewing food
- Avoiding fizzy drinks and alcohol.
- Drinking ample water or other fluids enriched with glucose and electrolytes
- Engaging in light post-meal activities, like walking.
If your symptoms are moderate to severe, your doctor may recommend drinking only liquids or eating well-cooked solid foods that have been processed into very small pieces or paste in a blender.
Blood Glucose Management
For gastroparesis caused by diabetes, maintaining appropriate blood glucose levels is crucial, especially to combat hyperglycemia, which can exacerbate gastroparesis. Strategies include:
- Adjusting insulin frequency or type.
- Administering insulin post-meals.
- Regular post-meal blood sugar checks, administering insulin as required.
Specific insulin instructions will depend on individual needs and gastroparesis severity.
Medication
Your doctor may prescribe medicines that help the muscles in the wall of your stomach work better. He or she may also prescribe medicines to control nausea and vomiting and reduce pain.
Several medications aim to enhance stomach muscle functionality include;
- Metoclopramide: Metoclopramide is used to enhance stomach muscle contractions and potentially augments gastric emptying, while also alleviating nausea.
- Domperidone: Domperidone is used as a muscle-contraction enhancer, available under a specialized U.S. FDA program.
- Erythromycin: Erythromycin is used to promote stomach muscle contraction and might enhance gastric emptying.
Several medications aim to reduce nausea and vomiting include;
- Antiemetics: Antiemetics is used to relieve nausea and vomiting. Examples include ondansetron, prochlorperazine, promethazine, bismuth subsalicylate, and diphenhydramine. These don’t impact gastric emptying.
- Antidepressants: Some, like mirtazapine, might combat nausea and vomiting but don’t necessarily improve gastric emptying.
- Pain Relievers: Non-narcotic analgesics can alleviate gastroparesis-associated abdominal discomfort.
Gastroparesis Lawsuits Against Ozempic, Wegovy, Rybelsus or Mounjaro
If you or a loved one have taken Ozempic, Wegovy, Mounjaro, or Rybelsus and subsequently developed symptoms of gastroparesis or any other gastric disorders, you may qualify for compensation.
Pharmaceutical companies have a responsibility to thoroughly test their products and provide adequate warnings about potential side effects. If they fail in this duty, they should be held accountable for the harm they cause.
If you suspect that your health complications are a direct result of using any of these medications, please do not hesitate to reach out. Our product liability lawyers are providing free consultations to assess the details of your experience and determine if you qualify for an Ozempic lawsuit, Wegovy lawsuit or Mounjaro lawsuit against the manufacturers.
Let us help you seek the justice and compensation you rightfully deserve. Contact us today to schedule your free consultation.
